Your own tooth is usually stronger and more efficient for biting and chewing.
Cleaning and maintenance of a natural tooth are much easier.
INFECTION AND INFLAMMATION
OF THE PULP
Infection or inflammation of the pulp can be caused by:
- Breakdown of a filling or crown
- A deep cavity
- Trauma
- Gum disease
- Crack or chip in the tooth
- Extreme wear
- Extensive dental work to the tooth
Symptoms may include pain, sensitivity to heat or cold, tooth discoloration, and swelling or soreness in the gum surrounding the tooth. To save the tooth, root canal treatment is needed when the pulp becomes severely inflamed or infected.
To improve the chance of success, root canal treatment should be stated as soon as possible. All root canal in the affected tooth must be treated. If the pulp of the tooth is not treated quickly, severe pain and abscesses (infections at the end of the roots) can occur. If an abscess is left untreated, infection can damage the bone surrounding the root.
Root canal treatment of the tooth involves:
A radiograph (x-ray film).
A local anaesthetic is usually given to block pain.
A sheet of latex, called rubber dam, used to isolate the tooth and keep it clean and dry during treatment.
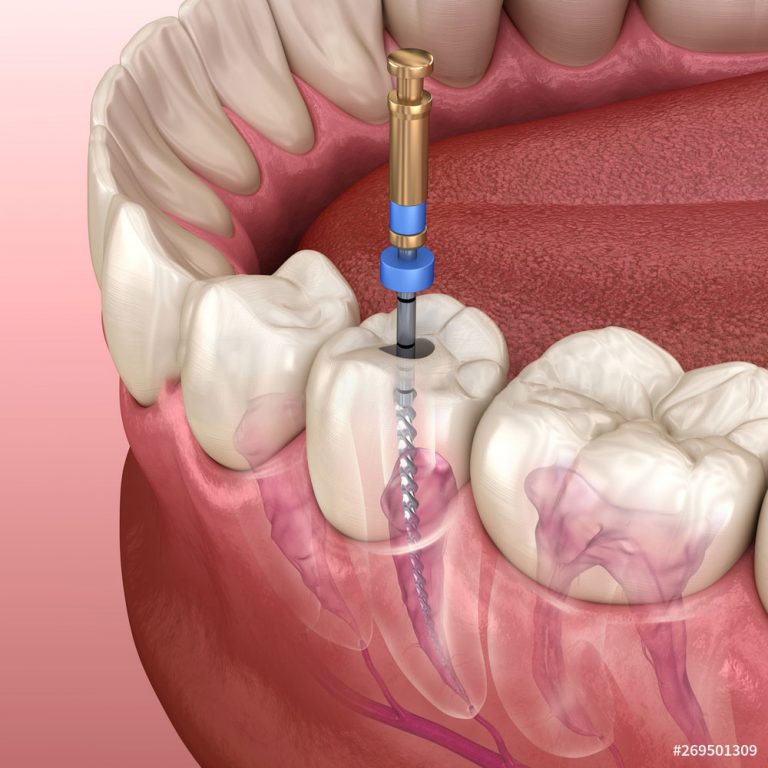
To reach the pulp, an opening through the roots is made with a dental drill. Using special instruments called files, your dentist will remove the inflamed or infected pulp. Each root canal is cleaned, enlarged and shaped. Anti-inflammatory and anti-bacterial medicines may be put inside the root canal to help stop the inflammation and infection.
If a severe abscess has formed at the root tip, oral antibiotics may be needed to treat the infection. You made need to make several visits to complete the treatment. A temporary filling will protect the inside of the tooth between visits. Pain or discomfort, if any, usually lasts no more than a few days, and will not be experienced by every patient.
Completion of treatment
To protect the inside of the tooth and prevent further infection, the roots canals are filled, and the pulp chamber is sealed. A post may be inserted inside the tooth if it lacks enough structure to support an artificial crown. At the jaw bone surrounding the treated tooth takes some time to heal completely, follow-up visits may be needed to see whether healing has been satisfactory. This is usually checked by examining the tooth and gums and by taking a radiograph. To help the healing process, you should continue to practice good hygiene, including brushing, flossing and regular check-ups
Fitting an artificial Crown
Your dentist may recommend that the tooth requires an artificial crown.
If your root canal treatment has been done by an Endodontist, then the Endodontist will recommend that you return to your dentist for the artificial crown. Usually an endodontically treated tooth has an increased risk of fracture without the protection of an artificial crown, so one should be fitted soon after treatment. Typically made of porcelain or gold, the artificial crown is needed to:
- Protect, strengthen and further seal the tooth
- Restore normal function and occlusion (the way the upper lower teeth contact each other when biting and chewing)
- Restore an acceptable cosmetic appearance.
Possible complications of root canal treatment
Loss of tooth: while root canal treatment can save the tooth, an important factor is the final restoration. Be certain to have your tooth restored completely, otherwise bacteria can re-enter the tooth and cause another infection.
Infection: infection in the damage tooth is likely to resolve completely once treatment is undertaken. The risks of re-infection are low. However, if the infection occurs again, the tooth may have to be treated again or removed.
Discolouration: in some cases, the treated tooth may lose its original whiteness and become darker. If a front tooth is affected, the person may feel unhappy about the tooth appearance. Discolouration can be treated by bleaching, or an artificial crown or veneer can be fitted.
Pain or Discomfort: Some people may continue to have pain or discomfort around the tooth during the following treatment. Your dentist or Endodontist may recommend a pain reliever. If the pain is severe or last more than a few days, tell your dentist or Endodontist. Additional treatment to the tooth may be needed.
Weakness: an endodontically treated tooth may not be as strong and durable as a normal tooth. (Molars), and this is why a crown is usually recommended.
Altered feeling: during and after treatment, the tooth may feel slightly different from the other teeth. This should disappear gradually.
File fracture: special metal files are used to clean the inside of the root canal. These instruments are very fine and occasionally break during use. Special procedures may be needed to remove the broken portion of the file, or you may be referred to an Endodontist.
Re-treatment: pain or infection may occur months or years after a tooth has been treated. This is usually due to further deep decay, trauma, a cracked tooth or a cracked filling that allows bacteria to enter the tooth and cause the infection. More endodontic treatment or extraction may be needed.